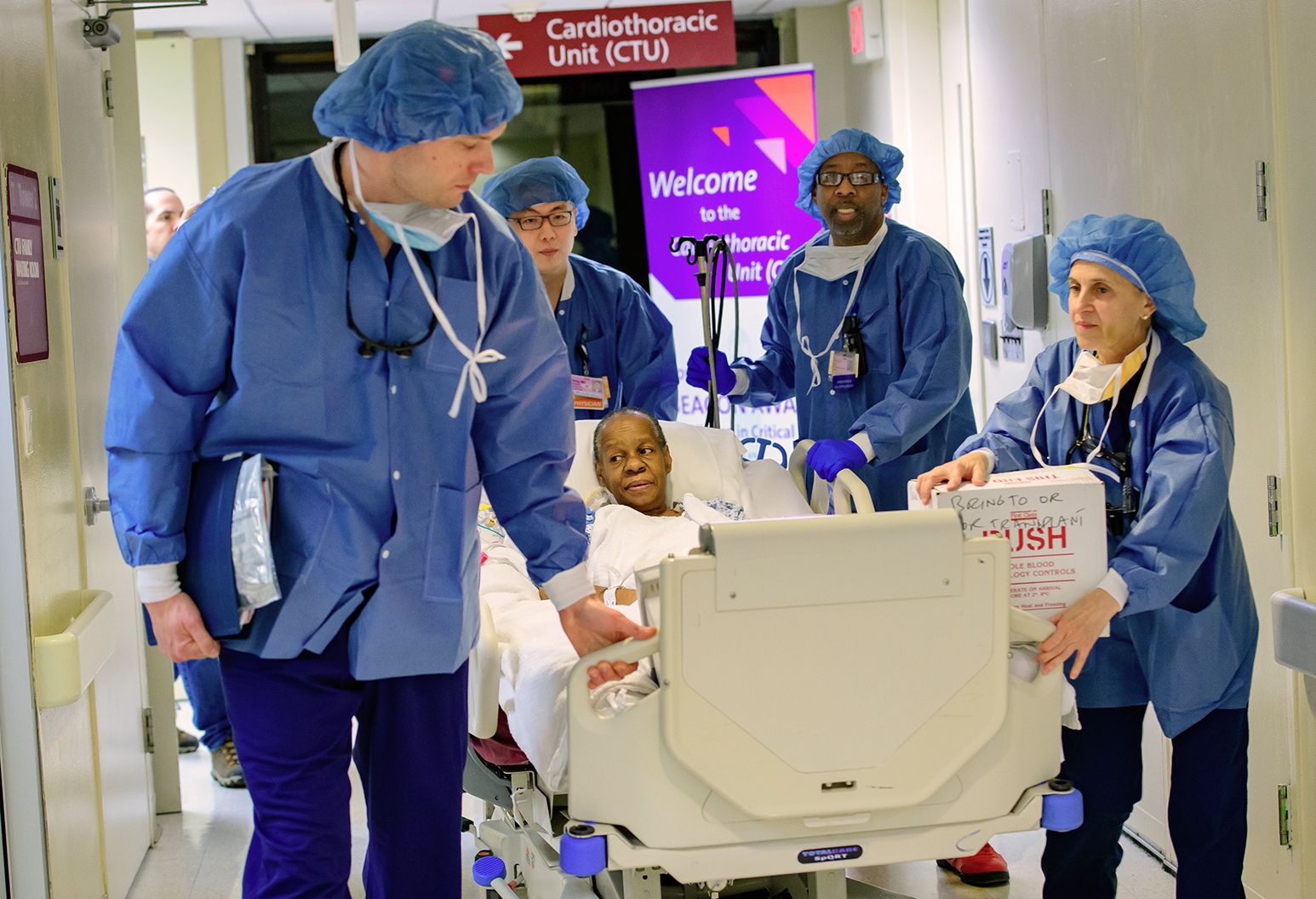
Lindsay Salguero-Lopez, 40, plans her days very carefully. A good habit to some, it’s a necessity of life for this resilient heart-and-lung failure patient, who has spent the last decade fighting an uphill battle to get to transplant.
Everyday activities like eating and bathing were exhausting events for Lindsay, who has lived with an un-repaired hole in her heart, known as a ventricular septal defect (VSD) since birth. The hole not only limited her lung capacity — making every breath a progressively painful choice — it robbed her of every activity or passion that brought her joy.
“I can only do maybe one thing a day,” said the Port Washington mother, who keeps her hair at shoulder length to reduce the effort it takes to maintain — a painful development for the former model. “Lately it’s been very, very hard just to breathe. To put on a shirt or pants is a struggle and I need help to do that.”
Long Island’s first lung transplant
That all changed on February 5, 2022, when she received a heart and double lung transplant at the Sandra Atlas Bass Heart Hospital at North Shore University Hospital, becoming the first person to receive a lung transplant on Long Island.
“Being the first operation of its type done on Long Island, it’s a great accomplishment,” said Aldo Iacono, MD, medical director for advanced lung transplantation at Northwell Health. “We have put together a team comprised of world-class physicians on both the surgical and medical side for both heart and lung, as well as nursing and physical therapy, ready to deliver state-of-the-art care within the Tri-state area, and I envision beyond that as well.”
Eight days prior, Lindsay fainted while grocery shopping with her husband and 16-year-old son — a rare trip into a public space during the pandemic. Her heart was essentially pushing against a “brick wall” caused by very high pressures in her lungs, said Zachary Kon, MD, Northwell’s surgical director of advanced heart failure and cardiac transplantation, as well as advanced lung failure and lung transplantation; and Lindsay’s surgeon. “And with that difficulty, her heart started to fail significantly.”
Lindsay told her husband to drive them home, before fainting a second time in the back seat of the car. He instead drove to North Shore University Hospital.
“It felt like somebody reached into my chest and started crushing my heart; I couldn’t breathe, couldn’t move, just felt terrible,” she said. “In my head I’m just praying, saying, ‘Please, please, God, I don’t want to die in the back of my car, in front of my son.’”
Near death, Lindsay’s only hope was a matching donor for both her heart and lungs. She had already waited three years on the United Network for Organ Sharing (UNOS) list, and many years before that. But two days after Northwell listed her, Lindsay’s luck finally changed.
“Taking a full breath is just amazing,” Lindsay said, one month after the late-night, life-saving surgery. “Every time I take a deep breath, it’s just overwhelming. I feel like crying every time I do something that I couldn’t do before.”
No longer limited to one activity per day, Lindsay has savored walks to the park with her husband and cooking with her family; and she hopes to go kayaking with her son this summer. On March 16, she returned to Northwell Health to thank the team of pulmonologists, cardiologists and surgeons who cared for her. They also included Samit Shah, MD, a cardiologist who continues to follow her care, and Arun Talwar, MD, a pulmonologist who has treated Lindsay since 1998.
“They have given me my life back,” she said, tears overtaking her words as she turned to thank her medical team. “They have given me the opportunity to continue to see my son grow, more years with my husband and my family.”
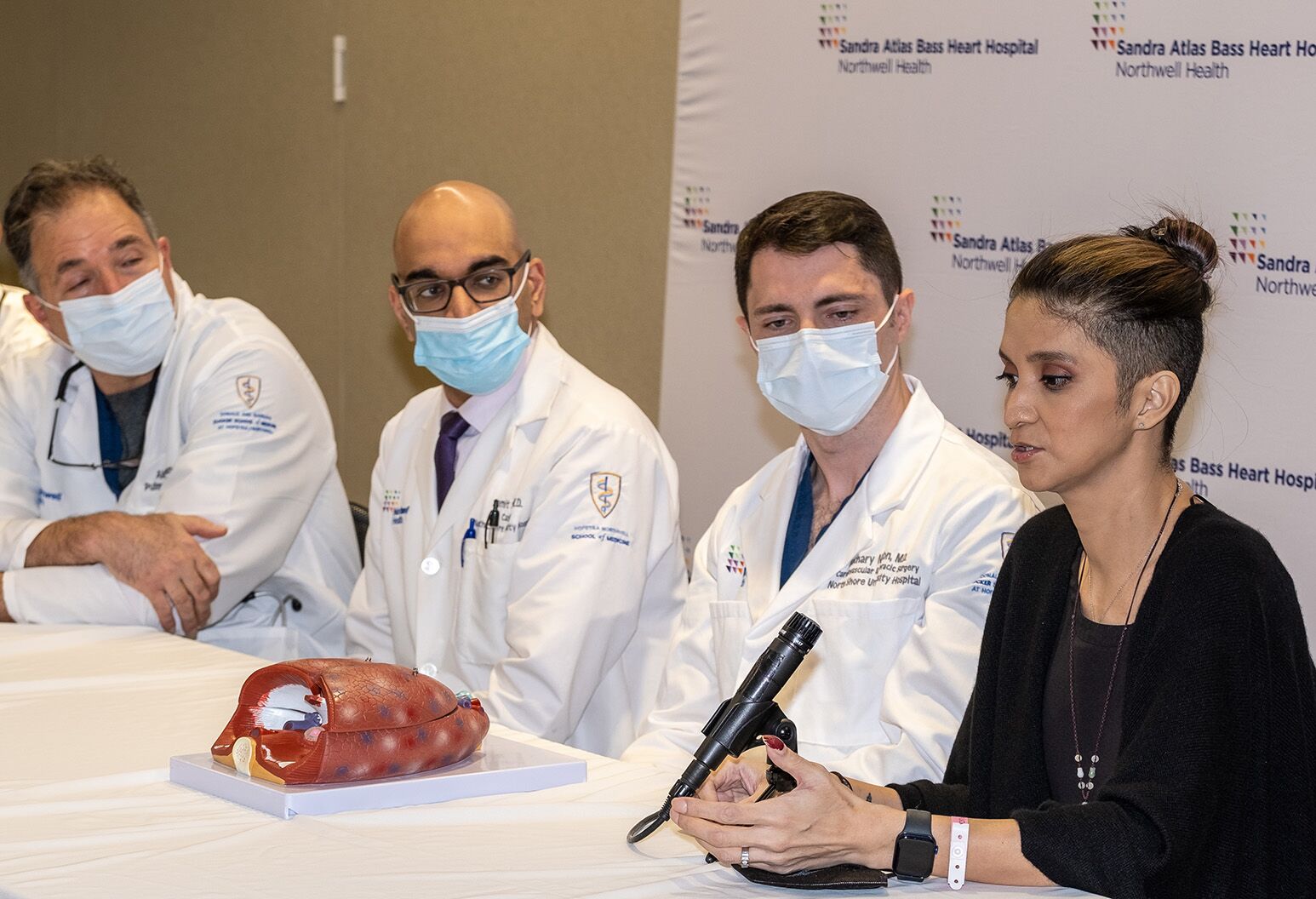
Keys to success after lung transplant
The moment that the cross-clamps were removed, Dr. Kon said, and blood started pumping through Lindsay’s new heart and lungs around 7 a.m. on February 5, “we knew that she was going to do really well: not only prolong her life, but get back to a good quality of life.”
Following lung transplantation, there are some key steps patients can take, which Dr. Kon said are equally important to the medical care they receive, to optimize their recovery:
Stay in shape: While de-conditioning pre-transplant is common and understandable, stay as strong as you can. One way to do this is to keep your nutrition up. For patients to get back to normal following transplant surgery usually takes several months. Be as active as you can and take full advantage of rehabilitation services available to you.
Take medications on time: Be a good steward of this organ. Anti-rejection drugs suppress the body’s immune response. While they help fight rejection — patients face the greatest risk of rejection in the first year — they reduce the body’s natural ability to fight off infections.
Keep appointments: Regular check-ins will catch problems early. And should anything out of the ordinary occur between visits, let your medical team know right away. Many times it’s a simple fix for a simple problem, especially if identified early. Before transplant, patients get a full assessment from a multidisciplinary team, which follows them through their recovery and years after. They include a:
- Cardiologist
- Cardiac surgeon
- Pharmacist
- Financial planner
- Neuropsychologists
- Palliative care clinician
- Social worker
- Psychiatry (if needed)
Get back into life: Frame of mind and a positive outlook can go a long way. Re-discover and celebrate all the victories that come from doing things you love, which you may have had to give up.
“I ask my patients not to thank me while they’re still in the hospital,” Dr. Kon said. “But when they get home and do whatever that thing is that they’ve been wanting to do for years, but haven’t been able to, I ask that they take a picture and send that to me.”
For Lindsay that was having dinner with her family without the use of oxygen; and when she’s gained her strength, kayaking with her son.
“Everything was so fast and so perfect; everything just worked out so well,” Lindsay said. “It’s nothing less than a miracle.”
VSD and Eisenmenger syndrome
Lindsay’s organ failure was the result of her lifelong struggle with a ventricular septal defect, a congenital condition that causes abnormal blood flow between the two lower chambers of the heart. Oxygen-rich blood meant to pump to the rest of the body escapes through the hole in the wall separating the left and right chambers, mixing with the oxygen-poor blood being pumped to the lungs. This excess blood flow causes high pressures in the lung arteries, which is pulmonary hypertension.
Eisenmenger syndrome is a potential long-term consequence of pulmonary hypertension, which forces the heart to work harder and can cause lung damage if left untreated.
“That also means blood without oxygen ends up going through her other organs and that is a big problem,” said Maria Avila, MD, medical director of cardiac transplant and mechanical circulatory support, Northwell Health. “Eventually, that will affect your kidney function, your liver function, your brain function, ultimately leading to multiple organ failure.”
Easily repaired when caught early in childhood, Lindsay went undiagnosed until age 6 and was left untreated until Lindsay’s mother, Alma, moved their family from Guatemala to the United States. Then 15 years old, the years of damage left transplant as the only option.
“My whole life has been full of scares, full of moments in the hospital where I’ve gotten the word, ‘There’s nothing else we can do,’” Lindsay said.
In 2019, extremely high pressures caused bleeding in her lungs. She was hospitalized and underwent five procedures that year to cauterize her lung vessels. That’s when Lindsay “went from ill to critically ill.”
“Having these high pressures for a long time makes the small vessels in the lungs very frail and patients with severe pulmonary hypertension tend to end up coughing up blood (hemoptysis), a life-threatening risk of pulmonary hypertension,” Dr. Avila said. “We see that a lot.”
When she fainted on January 27, 2022, the arteries between the heart and lung were so damaged that blood was now flowing in the opposite direction and going directly to the rest of her body without ever being oxygenated.
With her oxygen levels dipping below 50 – a normal range is 92-to-100 – her life was in jeopardy.
Expanding access to lung transplant services
There are currently just 73 lung transplant centers in the United States. Northwell’s new program will help to address the growing need for lung transplantation, notably as half of all lung transplant recipients at New York City hospitals traveled from Long Island, Queens, Brooklyn or Staten Island.
“Northwell being able to offer lung transplantation opens up options for the region and improves quality of life for their entire network of supporters on this life-saving health journey,” Dr. Kon said.
With the addition of lung, NSUH now offers world-class solid organ transplantation services for adult heart, kidney liver and lung. Cohen Children’s Medical Center in New Hyde Park also performs pediatric kidney transplants.